What the Hell Are We Supposed to Do With This New Research About Breast Milk?
Latest
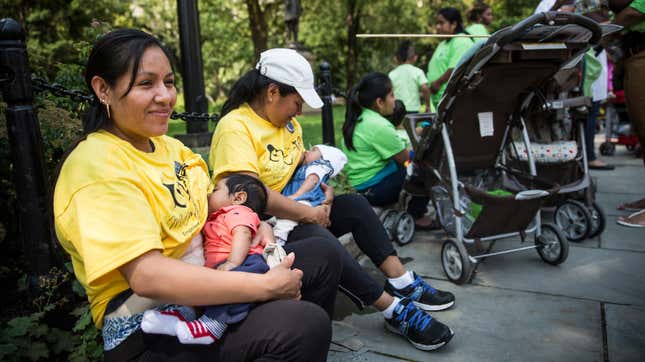
Brace yourself for another public debate about breastfeeding, because there’s new research that finds that, while breastmilk is really good for babies, it’s most beneficial when delivered directly from the breast. Pumping and bottling breast milk, a technique often used by nursing parents to navigate the monstrous time and logistical nightmare of breastfeeding, according to the study, does not pass on the same advantages. What parents should do with this crushing piece of information, well, researchers have fewer answers.
Breastmilk is full of essential bacteria that, per the New York Times, “colonize the infant’s gut, and could help set the course for the baby’s growing immune system and metabolism.” But researchers are still discovering the complicated relationships between antibodies, bacteria, and hormones that make breastmilk so important for an infant’s health.
Researchers in Israel recently discovered that one beneficial microbe, called bifidobacteria, grows faster as the the pregnancy develops in response to increases in progesterone. Bifidibacteria helps infants by digesting special sugars known as oligosaccharides, that babies cannot digest alone. While ample existing evidence suggests that breastmilk is beneficial for infants, new research led by Meghan Azad, a pediatric researcher and epidemiologist at the University of Manitoba, suggests that breastmilk consumed directly from the mother contains more of these beneficial microbes. The Times reports:
Dr. Azad and her colleagues studied 393 Canadian mother-infant pairs and found that pumped breast milk seems to be richer in some harmful bacteria, and has few bifidobacteria. Many variables can affect the quality of pumped breast milk, including the type of pump, how the milk is stored and the cleanliness of the bottles and nipples. Dr. Azad’s work suggests that direct contact between the mother’s breast and the baby’s mouth is important: When a baby nurses, some denizens of its oral microbiome may traverse back into the mother’s breast.
In other words, the benefits of breast-feeding may derive from myriad factors, including the many microbiomes in the mother’s body — in the breast milk and on the skin of the breast — and in the baby’s mouth and gut.
“I don’t want the message to be that expressed human milk is bad,” Dr. Bremer, a pediatric researcher at the Eunice Kennedy Shriver National Institute of Child Health and Human Development, told the Times. “It’s that there are other factors involved. When you disrupt that experience of baby sucking on the mom’s breast, what do you lose? Or what’s gained by that process? The science is more ripe now to start delving into those questions.”
From a scientific perspective, this is certainly an interesting discovery. But what, exactly, are nursing parents supposed to do with this research, given the altogether unreasonable expectations that already accompany breast feeding?
The American Academy of Pediatrics recommends that infants drink breast milk exclusively—whether by bottle or directly–until they are at least six months old. But in reality, only about one in four babies breastfeed exclusively for six months, possibly because of the numerous barriers. The United States has no federally mandated paid leave policy, meaning most new parents are not guaranteed paid time off to nurse their babies, and many businesses lack environments that would allow them to breast pump (Only about half of employers surveyed by the Society for Human Resource Management have an onsite lactation room for mothers; women working at one prison in Virginia even had to smuggle breast pumps in to use them). Insurance doesn’t adequately cover breastfeeding benefits, including lactation support providers or supplies.
And, while breastfeeding in public is legal, it’s heavily stigmatized, and women are discouraged from doing it. On top of all of that, retrieving information and assistance about breastfeeding is expensive and difficult.
As researchers continue to explore the wonders of the human body, lawmakers should focus on passing laws that support what we already know: new parents need way more support than they currently get.
 Keep scrolling for more great stories.
Keep scrolling for more great stories.

