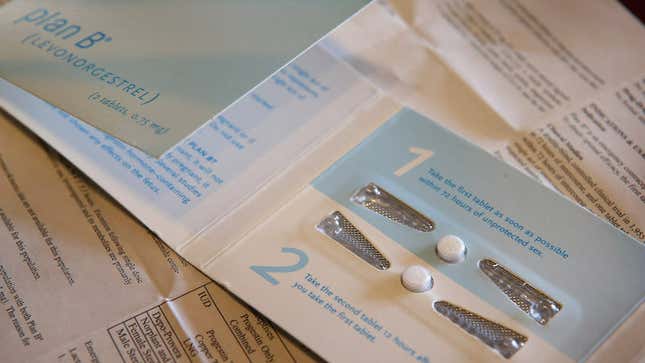

Emergency contraception (EC) is designed to prevent pregnancy. Some may choose it as their primary method of contraception, while others may use it in emergency situations only. Regardless of how you use it, it’s important to know all of your options and have the most accurate information, so you can make the best choice. There are so many myths about EC, so here are the facts.
EC is used after unprotected sex or after barrier protection (internal or external condom) fails. Some people may find that they haven’t been able to use their contraception method (like the pill or patch) or use fertility awareness as diligently as they planned.
There are a few methods of EC that are currently available—two in the form of a pill and the other in the form of an intrauterine device (IUD). Levonorgestrel (Plan B) and ulipristal (Ella) are both pill forms of EC that are currently available. Levonorgestrel may not work as well if you weight over 155 pounds, and is best if taken as soon as you determine that you need it (it may become less effective the longer you wait). Ulipristal is a better option for bodies of higher weight, but still may be less effective in those who weigh over 195 pounds. Ulipristal is equally as effective up to five days after unprotected sex. To be clear, having a higher weight doesn’t mean EC shouldn’t be taken at all—if you want to avoid pregnancy, it’s better to use EC than to not—it just means you should speak with your healthcare provider about your best options.
Levonorgestrel is available over-the-counter at a pharmacy and it’s also available on Amazon Prime; ulipristal is available with a prescription from a medical provider. Some college campuses now have EC pills accessible via vending machines, and California is working to mandate access to medication abortion on college campuses. It’s best to keep EC pills (and/or condoms) next to your bedside table, in your medicine cabinet, or in the suitcase you take on trips, so that you can take it as soon as it is needed (always remember to check the expiration date before taking the pill).
-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-

-








































